First of all, I live in Florida, which as you know refused Medicaid expansion and has thrown all sorts of roadblocks in front of ACA enrollment.
I am retired and drawing Social Security and VA Disability Compensation, so I do not need health insurance, but my wife and kids do.
I applied for them as soon as the ACA website went live and after a few stumbles, submitted my application well before the deadline.
Just prior to the deadline, Florida notified me that my family did not qualify because they are not U.S. citizens. All three have 10-year green cards. In Florida, this means you cannot receive any form of public assistance.
So, I gave up all hope of insuring them.
And then, I received an out-of-the-blue email from the Health Insurance Marketplace...
If you applied for a state health program, or you made changes to your state program information, you may get a notice explaining that you or someone on your application doesn’t qualify for Medicaid and Children’s Health Insurance Program (CHIP) in your state. Your notice will explain that your state application information was transferred to the Health Insurance Marketplace. When this happens, you may be able to get coverage through the Marketplace, and get help paying for health coverage and health services through:
A new tax credit that can be used right away to lower your monthly health insurance premium costs
Health plans specifically designed to lower your out-of-pocket costs
You’ll need the Application ID number that’s shown at the top of your state transfer notice from the Marketplace. Use this Application ID number to view, complete and submit your new transferred application in the Marketplace.
Cool. So, I re-applied with my new assigned application number (most of the fields were already filled in from my original application.)
The response... We qualified for very generous tax credits that made insurance possible for us. I followed the link to enroll and this is what I got...
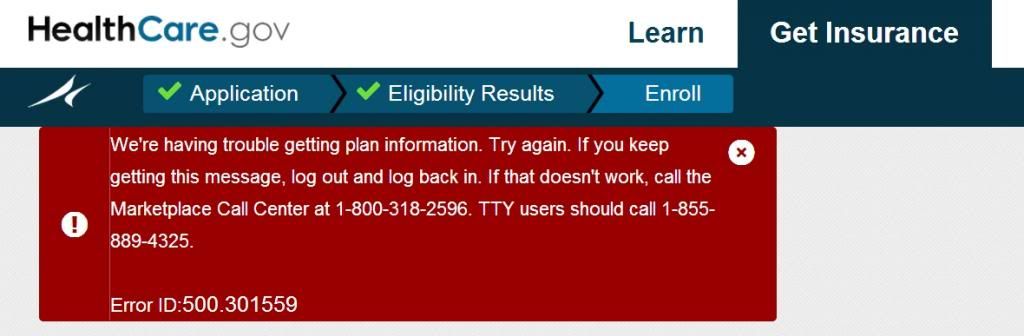
Bummer. I tried many times and received the same error message, so I called the Marketplace call center where I was told someone would call me back in 3-5 days.
That never happened, so I called them back. I was told that my case had been expedited and I would hear from them in 3-5 days.
Having already been downthat road, I started asking questions...
Is this because I live in Florida? ....NO.
Are others having the same problem? ....YES, MANY ARE.
The representative did not know how many people were affected, but from the sound of her voice (exhausted and exasperated, yet friendly), I suspect there may be a sizable number of folks in the states that are not ACA-friendly who are still waiting.
So, don't count me, but don't count me out, and don't stop counting total enrollees until the current bug has been fixed.


