With the passage of health care reform, many people are concerned about how it will affect their health care premiums. If health care premiums go down, then the reform succeeded; if they go up, then the effort was for nothing. So what in this bill actually controls the cost of health care premiums? I have seen many on DailyKos declare that there are no cost controls and that premiums will just keep going up. While it is true that the bill doesn’t mandate the prices of premiums or medical services directly, a number of provisions in the bill provide strong downward pressure on both premiums and medical cost, thus keeping cost under control.
Let's look at our current situation first. The basic driver for health insurance companies is for them to make a profit. There are three ways to increase this profit margin: reducing payouts, reducing administrative overhead, or increasing premiums. The first way, reducing payouts, can be accomplished by either putting downward pressure on medical costs or by denying claims. As we have seen in recent history, consolidation of health insurers has reduced competition, resulting in less downward pressure on premiums and less upward pressure on quality (ie, claim payout). As a result, it has become easier to raise premiums and deny coverage than to put downward pressure on medical costs. The financial gains from these have outweighed the side effect of additional administrative costs they create. With medical costs increasing due to lack of downward pressure and administrative costs increasing, the cost of premiums has ballooned. Here is a picture illustrating this effect:
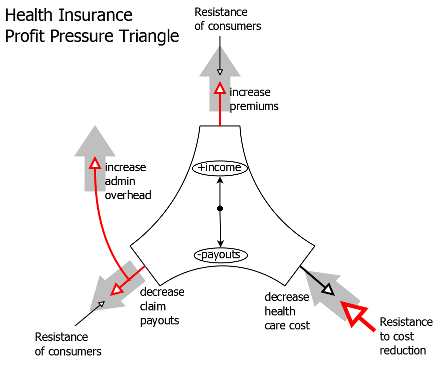
In order to solve the accelerating cost problem, the health care reform puts downward pressure on premiums, restricts the usage of claim denials, and restricts the proportion of costs that can go to administrative overhead. With these valves constricted, the remaining avenue for increasing margin is reducing health care costs. Some of the health care cost reduction is taken care of by the mandate, forcing uninsured people (who are disproportionately healthier [1]) back into the insurance pool. The rest will have to be taken care of by reduction in actual medical cost; health insurance companies will have to negotiate reductions in cost with providers. Here is a picture illustrating the new dynamic:
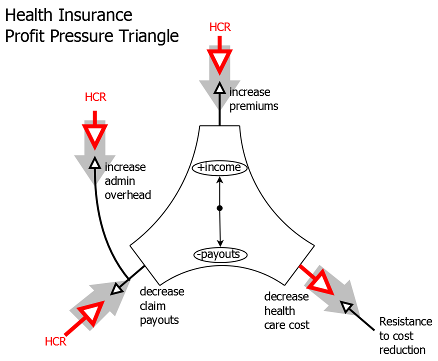
Health care reform uses several things to put downward pressure on premiums. The broadest tool is the creation of a proper health insurance marketplace, the exchanges. The bill includes several aspects that move health insurance much closer to the ideal of Perfect_competition, by increasing the number of sellers and increasing the information available to buyers. Every exchange is required to have at least two multi-state plans available, at least one offered by a non-profit entity (Sec 1334). States have the ability to form compacts to sell plans across state lines. The exchange will allow customers to rate plans and shop between them on an internet portal (Sec 1103), increasing transparency. With more availability and transparency of plans, competition will be higher and the plans will have better value for the cost.
The next tool to provide downward pressure on premiums is the ability of exchanges to completely block insurers from participating in exchanges if they raise premiums too high at any time between 2010 and 2014 (Sec 1003), and also gives exchanges the power to require plan certification when exchanges are in effect, part of which involves consideration of premiums (1311). This provides a backup for when an exchange doesn't get enough competition.
A third downward pressure on premiums is the excise tax on 40% of the cost of a premium that goes above $10,200 for single coverage and $27,500 for family coverage, starting in 2018 (Sec 9001). This creates a pretty strong cost barrier that everyone will try to avoid going past.
As for restricting the usage of claim denials, the reform accomplishes this by the banning of rescission (Sec 2712), and also requires plans to disclose denials in order to get certification (Sec 1311) and mandates a study on the rate of denial of coverage (Sec 1562).
Finally, for administrative overhead, the bill requires 85%/80% (large group/small group) of premiums to pay for medical costs (Sec 2718). With administrative overhead at 31% in the US [2], a cut down to 15%/20% is huge, and this goes into effect pretty soon, in 2011.
For the whole system to work, health care costs need to actually be cut, otherwise the premiums will continue to rise and we will be no better off. A large part of this cost reduction is the mandate. The key problem this provision solves is the insurance death spiral, where people jump out of insurance, thus making it more expensive, thus making more people jump out of insurance. There are those who believe the mandate isn't strong enough to actually get enough people to enroll. We just have to look at the Massachusetts health care reform to see the enrollment rates they experienced after their reform. The projected enrollment from their mandate was 225,000 in 2009 [3]; by September 2009, 430,000 had enrolled [4], nearly double the estimates. This indicates we will not really have a problem getting people to enroll.
So what about actually cutting medical costs? One option was to go the way of Canada, to restrict the supply of medical care to keep the cost down. Instead of following this path, the bill instead tries to attack medical costs in other ways. One of these ways is to demonstrate cost-reduction programs that can be exported to the whole system.
This is where the various programs to reduce cost in Medicare come in. Each method that successfully reduces cost, while at the same time not reducing quality, can be exported to the health care system at large. Non-Medicare providers don't have to do the experimentation - they can just implement the programs known to be successful. There are a lot of programs in the bill: tying hospital payment to hospital performance (Sec 3001), paying physicians based on the quality and cost of care they deliver (Sec 3007), adding penalties for conditions acquired in hospitals (Sec 3008), bundling payments (Sec 3023), reducing hospital readmissions (Sec 3025), and many others. The strongest measure it creates is the Independent Payment Advisory Board, which is given the authority to make propositions to Congress to reduce Medicare cost, which cannot be filibustered and can only be blocked if the Senate, House, and President agree.
There are a number of other cost reduction measures in the bill not related to Medicare that I won’t mention here. User deaniac83 gives explanations of cost control measures in "Beyond Insurance: Health care Cost Measures" (Part I, Part II, Part III).
So when do the different pieces start? The most immediate benefit will be the restriction on administrative overhead, which starts in 2011, next year. Also, exchanges will actually be able to block insurers from exchanges based on their premium increases starting in the year 2010, so insurers have to justify their increases every year before the exchanges even begin. The internet portal allowing access to coverage information was put into effect on enactment, so we should see better information for consumers starting soon.
The remaining large piece, a competitive market in the exchanges, won't arrive until 2014. At that point, the market will require less smack-downs by the exchanges due to higher competition providing a more natural downward pressure on premiums. Also, the Medicare cost reduction programs, which kick in during years between 2012 and 2015, should start showing results. Additionally, plans will start requiring an analysis of denial of care in order to be certified for the exchange, so denials should decrease. But even until the exchanges arrive, several components will combine to provide a good amount of cost control on health insurance premiums.
So where do we go from here? In order for us to realize the benefits of the health care reform, we need to make sure that the health care industry as a whole adopts the cost-saving methods demonstrated by the Medicare pilot programs. Due to institutional resistance to change, we may not see automatic adoption. We don’t know yet which ones will have the most savings, but when we do, we may need to push for legislation that mandates their adoption in the rest of the system; otherwise, cost may spiral out of control. This is where groups from both the left and right can work together, pushing for successful cost control programs: people from the left wanting the health care reform to succeed, and people from the right wanting costs to be contained. Let’s make health care reform a reality.
Resources
Bill summary: http://dpc.senate.gov/...
[1] http://aspe.hhs.gov/...
[2] http://www.pnhp.org/...
[3] http://www.boston.com/...
[4] http://www.kff.org/...


